When evidence-based design collides with conventional wisdom, the outcome will sometimes be disruptive.
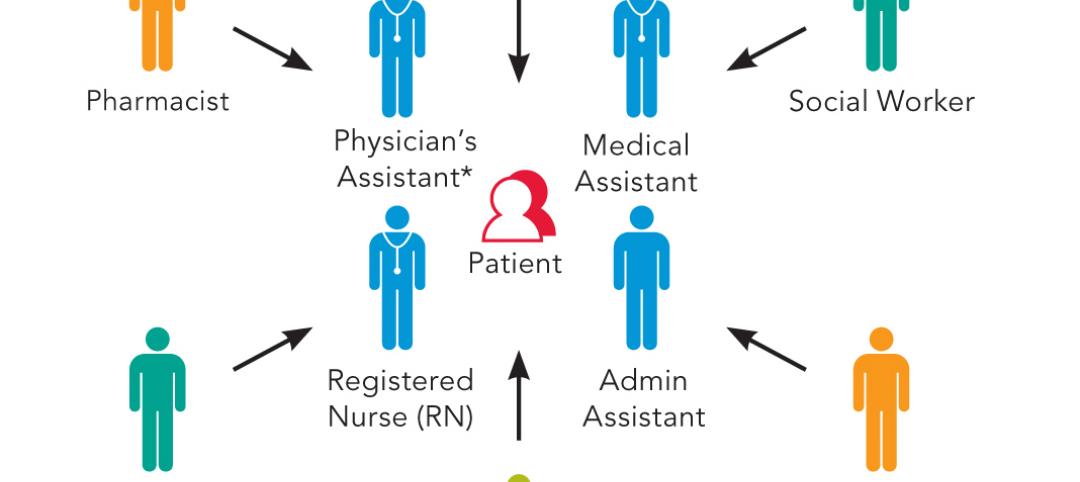
Take, for example, the generally accepted advantages in patient care and observation related to decentralizing nurses’ stations in hospitals, which is becoming standard practice for healthcare clients and their AEC partners.
A recent evaluation of a renovated Missouri hospital, conducted by University of Kansas faculty members, raised questions about the impact of decentralization on patient satisfaction and the communication among nursing teams within the facility.
The St. Louis-based architectural firm Lawrence Group retained the Institute for Health + Wellness Design (IHWD) at KU’s School of Architecture, Design, and Planning to provide a third-party review of the firm’s 2014 remodeling of the orthopedic unit at SSM St. Mary’s Hospital in Jefferson City. That healthcare system was about to embark on an expansion of its St. Joseph Hospital West in Lake St. Louis.
Lawrence Group is an affiliate member of IHWD.
The Institute assessed the unit using an evidence-based design checklist developed by the nonprofit Center for Health Design in California. Its survey included a “space syntax” evaluation that generated a heat map, which showed how the unit’s layout might affect patient satisfaction.
“We wanted to see does moving into a new facility improve patient satisfaction scores, which is one of the most important things for hospital owners today,” said Hui Cai, Assistant Professor at KU, who with Professor Kent Spreckelmeyer and Frank Zilm, IHWD’s chairman, presented findings from the Institute’s nursing unit study at the Healthcare Design Conference 2016 in Houston last November.
The study found, perhaps not surprisingly, that the facility itself showed “statistically significant increase[s]” in scores after the renovation. But patient-quality scores mostly stayed the same, and one score—nurses’ responses to patient calls—actually dropped slightly.
The Institute hypothesizes that decentralization was the culprit, due to the physical distance and visual disconnection of decentralized nursing unit design, which necessitates that nurses must move farther to get from station to station. The Institute suggests these distances might be an impediment to interaction among nurses that might also delay responses to patients.
“This design trend needs to be further investigated before it is accepted as standard for every hospital,” said Cai. “We have to see how to modify the design to achieve balance between shorter walking distance, better patient surveillance and better staff communication and collaboration.”
This is one of the first research studies to link decentralized nurse station design with organizational performance and patient outcomes. The Institute has conducted a second phase of study to evaluate further the degree to which decentralized design affects nurses’ teamwork and patients’ perception of care. In late 2017, IHWD plans to present and publish the results of this study, which included a second hospital, the University Medical Center of Princeton at Plainsboro, N.J.
Related Stories
| Dec 1, 2014
How public-private partnerships can help with public building projects
Minimizing lifecycle costs and transferring risk to the private sector are among the benefits to applying the P3 project delivery model on public building projects, according to experts from Skanska USA.
| Nov 25, 2014
Emerging design and operation strategies for the ambulatory team in transition
As healthcare systems shift their care models to be more responsive to patient-centered care, ambulatory care teams need to be positioned to operate efficiently in their everyday work environments, write CannonDesign Health Practice leaders Tonia Burnette and Mike Pukszta.
| Nov 20, 2014
Lean Led Design: How Building Teams can cut costs, reduce waste in healthcare construction projects
Healthcare organizations are under extreme pressure to reduce costs, writes CBRE Healthcare's Lora Schwartz. Tools like Lean Led Design are helping them cope.
| Nov 18, 2014
5 big trends changing the world of academic medicine
Things are changing in healthcare. Within academic medicine alone, there is a global shortage of healthcare professionals, a changing policy landscape within the U..S., and new view and techniques in both pedagogy and practice, writes Perkins+Will’s Pat Bosch.
| Nov 14, 2014
Haskell acquires FreemanWhite, strengthens healthcare design-build business
The combination expands Haskell’s geographic presence by adding FreemanWhite’s offices in Chicago, Charlotte, Nashville, and San Diego. FreemanWhite will retain its name and brand.
| Oct 30, 2014
CannonDesign releases guide for specifying flooring in healthcare settings
The new report, "Flooring Applications in Healthcare Settings," compares and contrasts different flooring types in the context of parameters such as health and safety impact, design and operational issues, environmental considerations, economics, and product options.
| Oct 30, 2014
Perkins Eastman and Lee, Burkhart, Liu to merge practices
The merger will significantly build upon the established practices—particularly healthcare—of both firms and diversify their combined expertise, particularly on the West Coast.
| Oct 21, 2014
Passive House concept gains momentum in apartment design
Passive House, an ultra-efficient building standard that originated in Germany, has been used for single-family homes since its inception in 1990. Only recently has the concept made its way into the U.S. commercial buildings market.
| Oct 21, 2014
Hartford Hospital plans $150 million expansion for Bone and Joint Institute
The bright-white structures will feature a curvilinear form, mimicking bones and ligament.
| Oct 16, 2014
Perkins+Will white paper examines alternatives to flame retardant building materials
The white paper includes a list of 193 flame retardants, including 29 discovered in building and household products, 50 found in the indoor environment, and 33 in human blood, milk, and tissues.