The occasional pleasant surprise is always nice, but an unanticipated tornado is rarely greeted with enthusiasm. Most of us prefer a relatively predictable future with adequate warning when the occasional storm heads our way.
Unfortunately, our current political drama has made our healthcare clients view the future of their business environment in much the same way most of us approach the latest weather report. We want to stay abreast of the latest news, but what we hear is greeted with skepticism.
Just as very few of us would bet a significant amount of our wealth on the reliability of weather predictions, our healthcare clients are struggling with how best to approach long-term planning when our national healthcare policy seems to change with the nightly news cycle.
Within this rancorous political environment and the uncertainty that it imposes on the healthcare industry, architects are asking themselves how they can best serve their healthcare clients with decisions that have significant cost and long-term implications.
Our advice to fellow architects and clients alike is to focus on what you know and avoid speculative investments.
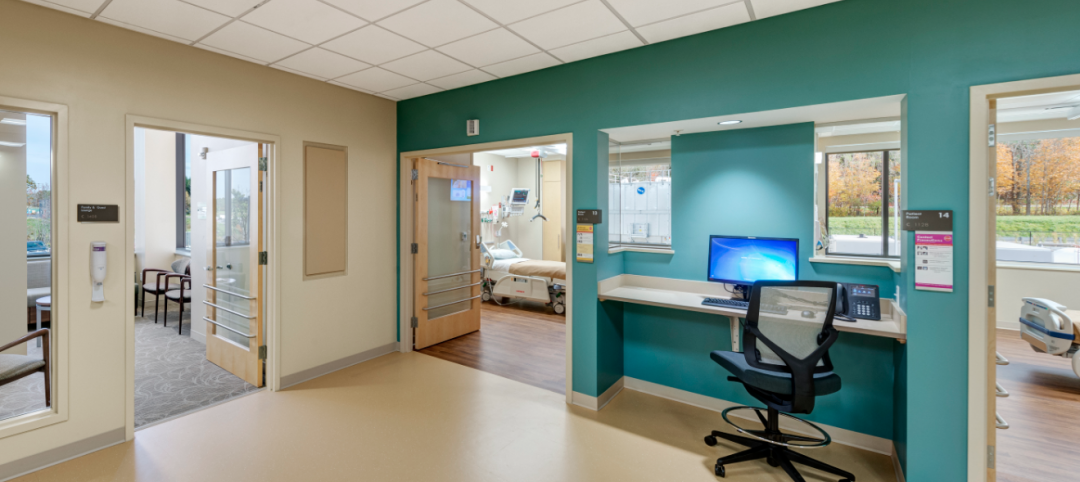
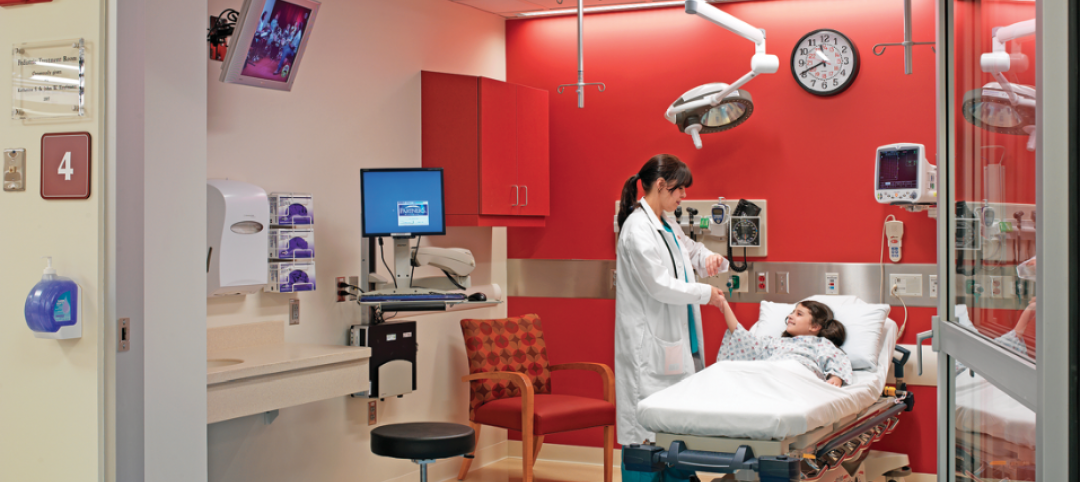
We know, for example, that most of the nation’s healthcare infrastructure is aging, with many hospital campuses occupied by buildings that are ill-suited to meet the demands of modern healthcare.
We know that we have an aging Baby Boomer population that will require care and treatment for chronic problems that accompany old age. We also know that they are living longer than their parents did.
We’re aware, too, that the demographic and financial composition of the country is evolving. We know that many of the rural areas of the country are poorly served and lack adequate healthcare services. We also know that many urban areas have inadequate or poorly distributed trauma services.
These realities provide direction for where healthcare providers might make meaningful and defensible investments—at least until the political seas calm and the way forward is a bit more predictable.
For healthcare architects, these realities also offer potential opportunities for marketing strategies that can be tailored toward the types of projects that might surface during this stressful period. Projects could include the modernization of existing facilities, conversions from semi-private rooms to private rooms, or energy system upgrades that reduce operating costs.
More proactively, healthcare planners and designers might consider bundling services that are directed toward strategically assisting their clients with assessing opportunities within their existing healthcare campuses—opportunities that could improve operational efficiency, space utilization, and throughput.
Architects may be as ill-equipped to resolve the healthcare policy turmoil as everyone else, but healthcare designers are very well positioned to assist their clients strategically with insight and creativity—not only to navigate the stormy waters that are currently roiling the industry, but also to make meaningful interventions that provide long-term value to the communities they and their healthcare clients serve.
Related Stories
Healthcare Facilities | Oct 23, 2015
Mortenson study: Healthcare providers optimistic, but want changes to Affordable Care Act
The 2015 Mortenson Healthcare Industry Study found that 76% of providers are at least optimistic about the future of healthcare, but eight out of 10 would like to see changes made to ACA.
Healthcare Facilities | Sep 29, 2015
The ever changing physician real estate market
In the United States, the environment where outpatient healthcare is being delivered is as dynamic and diverse as the more high profile office and retail markets, writes CBRE Healthcare's Nelson Udstuen.
Healthcare Facilities | Sep 21, 2015
5 reasons healthcare organizations are implementing finish standards on construction projects
The desire for improved patient satisfaction, staff retention, and turn-key maintenance are among the top reasons more healthcare groups are implementing finish standards in their spaces, according to VOA Associates' Lauren Andrysiak.
Healthcare Facilities | Sep 11, 2015
Health Product Declaration Collaborative releases updated HPD Open Standard – Version 2.0
Advances transparent disclosure of building product contents
Healthcare Facilities | Aug 28, 2015
Hospital construction/renovation guidelines promote sound control
The newly revised guidelines from the Facilities Guidelines Institute touch on six factors that affect a hospital’s soundscape.
Healthcare Facilities | Aug 28, 2015
7 (more) steps toward a quieter hospital
Every hospital has its own “culture” of loudness and quiet. Jacobs’ Chris Kay offers steps to a therapeutic auditory environment.
Healthcare Facilities | Aug 28, 2015
Shhh!!! 6 ways to keep the noise down in new and existing hospitals
There’s a ‘decibel war’ going on in the nation’s hospitals. Progressive Building Teams are leading the charge to give patients quieter healing environments.
Mixed-Use | Aug 26, 2015
Innovation districts + tech clusters: How the ‘open innovation’ era is revitalizing urban cores
In the race for highly coveted tech companies and startups, cities, institutions, and developers are teaming to form innovation hot pockets.
Healthcare Facilities | Aug 19, 2015
5 brand-building strategies in the outpatient environment
No longer coasting off of reputation, leading organizations are using new ambulatory care centers to re-brand for the future of healthcare, writes CannonDesign's Jocelyn Stroupe.
Healthcare Facilities | Aug 18, 2015
Transforming the patient-clinician experience in retail healthcare: 5 'flips' to consider
Flip the Clinic is a Robert Wood Johnson Foundation project invented to transform the patient-clinician experience. In their language, “flips” are actionable ideas for change, writes Gensler's Tama Duffy Day.